Introduction
Clinically, muscle tone is assessed by judging the resistance of a patient’s limb to passive stretch. Damage to the descending motor pathways that terminate in the spinal cord can cause hypertonia, and therefore In stroke, lack of afferent sensory information (proprioception) and miscommunication between the cerebral cortex (motor and sensory regions) with other subcortical regions cause a dysregulation in the control of muscle tone. This dysregulation results in an increased resistance to passive movement or in other words hypertonicity (or spasticity).
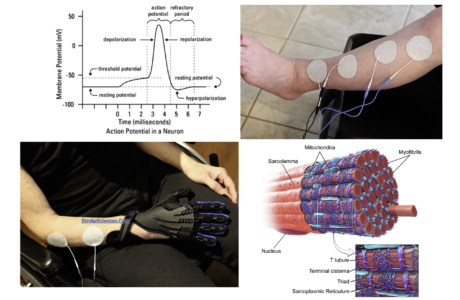
Two main characteristic signs of hypertonicity is the clasp-knife phenomenon and clonus. When first stretched, a hypertone muscle provides a high level of resistance to the stretch and then suddenly yields, much like the blade of a pocket knife. Hyperactivity of the stretch reflex loop is the reason for the increased resistance to stretch in the clasp-knife phenomenon. On the other hand, clonus refers to a rhythmic pattern of contractions (3-7 Hz) due to alternate stretching and unloading of the muscle spindles in hypetone or spastic muscles¹.
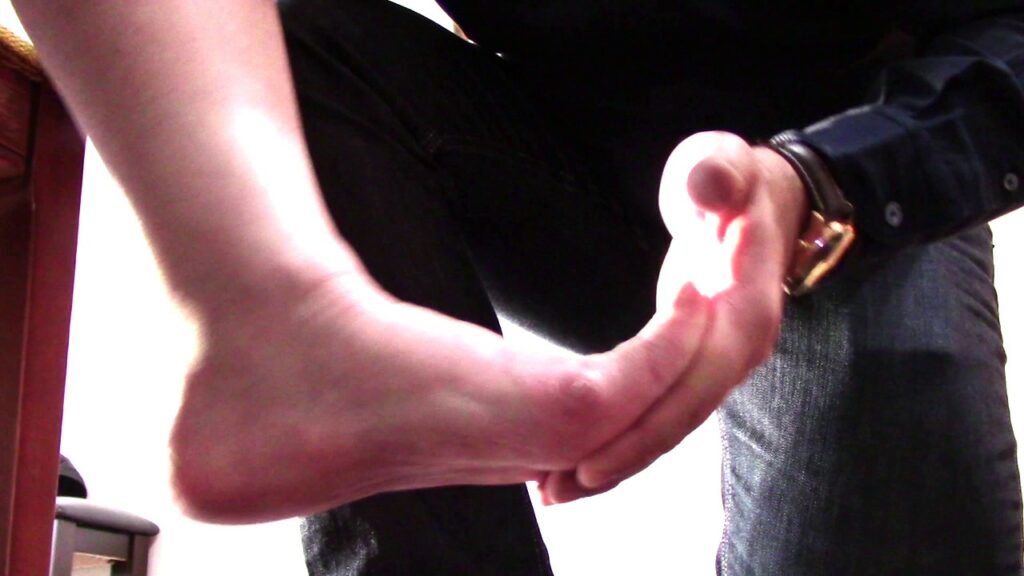
Clonus can be demonstrated in the flexor muscles of the leg by pushing up on the sole of a patient’s foot to dorsiflex the ankle. If there is a damage to descending upper motor neuron pathways, holding the ankle loosely in the position generates rhythmic contractions of both the gastrocnemius and soleus muscles² as shown in the video.
Significance
The presence of clonus is indicative of a damage to the descending upper motor neuron pathways in stroke or spinal cord injuries.
References: